The AIDS epidemic in the United States officially began on June 18, 1981, when the U.S. Centers for Disease Control and Prevention (CDC) reported a small grouping of Pneumocystis carinii pneumonia (now classified as Pneumocystis jiroveci pneumonia) cases in five gay men in Los Angeles, California. Considered to be a pandemic, Acquired Immunodeficiency Syndrome (AIDS) claimed between 2.8 and 3.5 million lives worldwide in 2004, according to the World Health Organization (WHO). Although there are treatments for AIDS, there is no cure, nor a vaccine.
 HIV/AIDS distinction
HIV/AIDS distinction
AIDS is a collection of symptoms and infections derived from the collapse of the immune system, produced by the infection of the Human Immunodeficiency Virus (HIV). The virus, which can remain latent for up to 10 years, is the underlying cause of AIDS. The two species of HIV infecting humans (HIV-1 and HIV-2) originated in an African chimpanzee subspecies and an Old World monkey of Guinea Bissau, Gabon, and Cameroon, respectively. Originally thought to have been transferred through sexual intercourse with those primates, epidemiologists theorize the disease actually spread when hunters came into blood contact with primates infected with SIV, which is the form HIV takes in infected sub-Saharan monkeys.
Progressively destroying the body's ability to fight infections and certain cancers, HIV kills or damages cells that aid the body’s immune system and enables the introduction of life-threatening diseases. AIDS patients contract opportunistic infections through viruses or bacteria that cause such diseases as Kaposi Sarcoma, tuberculosis, and a host of unusual infections and cancers. Those with HIV who did not exhibit symptomatic diseases that the U.S. Centers for Disease Control and Prevention associated with AIDS, were initially identified as having AIDS-related Complex (ARC). Broader definitions, introduced by CDC in 1987, included neurological symptoms, wasting syndrome, and more common infections that redefined those with ARC to patients with AIDS.
Recent studies indicate that the CD4+ (or “Helper”) T-Cells, which serve as immune system aids in its fight against deviant or infected cells, are destroyed by the HIV virus. The decrease in the number of those cells that serve as "middlemen" in the immune response, results in a weakened immune system that is more susceptible to immunodeficiency diseases. Although only a small number of Helper T-Cells are actually infected with HIV at any given time, researchers have been able to detect an ongoing cycle of death and infection of new target cells during the course of the disease. If the CDC revises their AIDS definition to include those with lowered Helper T-Cell counts, it would result in the doubling of the estimates of those with AIDS. Antiretroviral drug therapies with protease inhibitors, which reduce HIV in the blood and increase the number of Helper T-Cells the immune system needs to fight off infection, are taken in conjunction with other drugs to slow the progression to AIDS. The multi-drug therapy approach has led to a 70-percent drop in the number of people susceptible to opportunistic infections, or those who have died from AIDS.
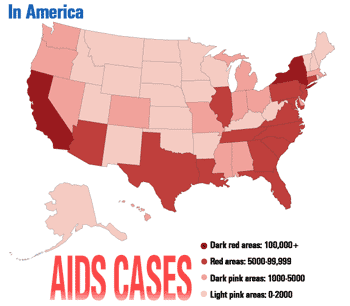
It has been determined that the transference of HIV is caused through anal, vaginal, or oral sex; blood transfusions; the use of contaminated needles in a health care setting and through drug injection; or from mother to child during pregnancy, childbirth and breastfeeding. In Africa, it also is known to be transmitted during child circumcision with an instrument tainted with the HIV virus. Initially, HIV was found exclusively in sexually active heterosexuals in Africa.
History of AIDS in America
Originally thought to have been carried into the U.S. by French-Canadian flight attendant Gaetan Dugas, epidemiologists’ research indicates such distinct strains of the disease could not have been introduced by one person. Their research also indicates its entrance date was actually around 1968, which does not coincide with the Dugas introduction story that appeared in And the Band Played On, written by San Francisco Chronicle reporter Randy Shilts. The first known case of HIV was found in a person who died in the Congo in 1959.
First thought to have only affected the male homosexual population, the term GRID or Gay-related Immunodeficiency Disease was originally proposed for the syndrome. Instead, a less controversial and more neutral term called AIDS was adopted. Early reports of unusual infections and cancers in otherwise healthy young homosexual men began to surface in San Francisco, California, and New York City in 1981. Findings of an atypical pneumonia and a cancer in homosexual men — previously found only in elderly Mediterranean men — was the subject of the first report of its kind in the Morbidity and Mortality Weekly Report. During that year, 234 AIDS deaths occurred in the U.S. The following year 853 known deaths occurred.
Early research found that persons with those infections also suffered from hepatitis B acquired in bathhouses. Due to many obscure extraneous factors, common trends for the disease were not accurately diagnosed, and efforts to control its spread resulted in bathhouses in San Francisco, and elsewhere, to be closed. One suggestive trend was the use of such drugs as inhalant stimulants in affected men. It was later found that the carrier of such infections was blood. Infected blood was traced to those who used intravenous drugs or were the recipients of blood or blood products from homosexual male donors who were either dying, or had died, of AIDS. When the first antibody test for HIV became available, it was found in frozen blood samples that had been saved from a hepatitis B study in the late 1970s, showing the parallel to hepatitis B.
In 1983, France isolated the HIV virus that caused AIDS. By the end of that year, 2,304 deaths in the U.S. were attributed to AIDS. Politically kept quiet, President Ronald Reagan still had not mentioned the word AIDS in public until September 17, 1985, in response to reporters questions regarding the subject. By the end of that year, known deaths jumped to 5,636, including film star Rock Hudson. In President Reagan’s February 6, 1986, Message to the Congress on America’s Agenda for the Future, he mentioned AIDS. During that same year, U.S. Surgeon General Everett Koop published a report on AIDS that called for sex education.
With the introduction of Glaxo Wellcome’s AZT (zidovudine Retrovir) in 1987, which became the first anti-HIV drug approved by the U.S. Food and Drug Administration (FDA), a number of other drugs followed over the next nine years. From humble treatment beginnings with such anti-HIV drugs as AZT, with the recommended dosage of one 100mg capsule every four hours around the clock,* over the years multiple drug therapies proved to be more effective than single-drug therapies. That same year, President Reagan gave his first “major speech” on AIDS before the College of Physicians in Philadelphia, Pennsylvania, calling it “public enemy number one.” Vice President George H.W. Bush was ridiculed for calling for mandatory HIV testing.
AIDS activist groups sprang up around the country in the latter part of the 1980s and have impacted the treatment and continued research for a cure and vaccine for HIV/AIDS. The People with AIDS Coalition, established in 1986, initially focused on the healing methods and alternative therapies for the treatment of AIDS. The group later broadened their focus to include the needs of the HIV/AIDS community. The AIDS Coalition to Unleash Power (ACT UP), established in March 1987, has been instrumental in furthering the research and development of a cure for the AIDS epidemic in the United States. On March 24, 1987, just a few weeks after its establishment, ACT UP demonstrated on Wall Street, in New York City, to increase public awareness of the high cost of the anti-HIV drug AZT. As a result, the FDA shortened the drug approval process by two years. After two years of protests, Burroughs Wellcome lowered the prescription cost of AZT by 20 percent. The previous year, the FDA had approved the importation of non-approved treatment for AIDS sufferers.
Many advances in drug therapies and social awareness of HIV and AIDS were made in 1996 when Dr. David Ho, Time Magazine’s Man of the Year, shifted the focus of AIDS research from later stages of the illness to early stages of HIV infection. Ho’s research, yielding a “cocktail” of antiretroviral drugs that combat the ravaging effects HIV has on the immune system, may lead to a future cure for the virus. In addition, California and Arizona voters passed propositions allowing for the medical use of marijuana, and 34,947 Americans died of AIDS that year.
Media coverage of the AIDS epidemic in the U.S. has waned over the years, according to a survey published in 2004. Stories about HIV and AIDS were relatively few during the peak years of the 1990s, but stories increased with basketball star Magic Johnson’s announcement of his HIV status in 1991. The introduction of combination therapies spurred a resurgence of media coverage between 1996 and 1997. In May 2004, the news media publicized the HIV outbreak among the U.S. porn industry as five actors became HIV-positive. A billion-dollar industry, porn stars were thereafter frequently monitored for HIV.
Research for a cure
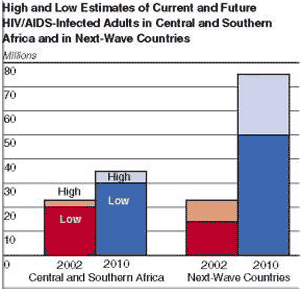
With more than 39 million adults and children infected worldwide, HIV is one of the most devastating threats to human health. As a result of HIV’s ability to reproduce itself so readily in the blood, where it creates slightly different strains with each reproductive cycle, a cure has eluded researchers since the epidemic was announced in 1981. The introduction of protease inhibitors and other anti-HIV drug therapies has exerted a significant impact on the immune system’s ability to fight off the disease, but it has not succeeded in killing off the inactive HIV-infected cells. According to recent research performed at a Texas laboratory, some of those latent and hidden cells have been uncovered with valproic acid and then killed using an increased dosage of conventional HIV drugs. The success of that form of experimental treatment has led to a 75-percent drop in cells providing refuge to latent HIV cells, but the completion of their testing and evaluation is not due to be completed for at least another 10 years. Since the virus increases exponentially once it becomes active, every HIV-infected cell must be extinguished to prevent the spread of HIV.
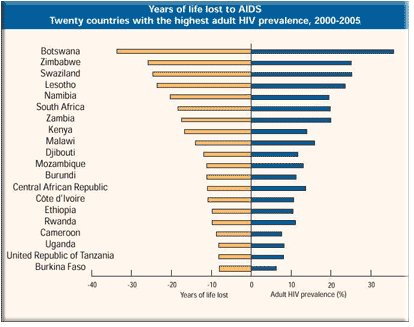
With an introduction of two-drug therapies in clinical trials, there was a 50-percent time increase before the progression of AIDS. With the recent introduction of three-drug combination therapies, that progression has been slowed another 50 to 80 percent when compared with the two-drug treatments. While those results have been quite stunning in patients where treatment is available, the spread of HIV in African, South American, and Asian countries continues to pose serious threats to the physical welfare and economy of those nations without them.
Advancements have been made in preventing transmission of HIV from mother to child, using nevirapine, despite news stories distorting the actual facts, according to an April 2005 study published by the U.S. Institute of Medicine. Other advances include the FDA-approved OraQuick Advance Rapid 1/2, which is a rapid HIV test that uses oral fluid, and the first not to require a whole blood specimen. Results can be seen after only 20 minutes, with an accuracy of 99.8 percent in clinical tests. According to a survey done in June 2005, an estimated $682 million dollars is spent on AIDS vaccine research annually, but there is no vaccine for HIV.
Funding battles for HIV/AIDS research
Lack of financial support by the world’s richest nations is the fundamental reason why WHO’s attempts to treat three million people in 2005 is failing. With the cost of drug therapies ranging from $850 to $1,150 per year internationally, treatment of HIV and AIDS has placed a massive financial responsibility on those countries. For the 2006 budget proposal, $3 billion or 14 percent of the total $21 billion budget will be spent domestically on AIDS research. With 13,000 worldwide infected with HIV every day, the cost of today’s most advanced drugs only keep the virus from running out of control. With more than $12 billion needed to adequately address HIV/AIDS prevention, care, and support in low- and middle-income countries, only $6 billion has been spent. There were between 1.04 million and 1.185 million people living in the U.S. with HIV/AIDS in 2003. Proposed funding for domestic research, care, prevention, and treatment amounted to $17.1 billion.
U.S. funding of $15 billion from President George W. Bush’s initiative is called the President’s Emergency Plan for AIDS Relief, or PEPFAR. Beginning with its first installment in January 2004, PEPFAR’s plan was to aid mostly African countries, but also Guyana, Haiti and Vietnam. Its goal was to treat 200,000 AIDS sufferers by June 2004. According to its reports for the end of March 2005, the fund claimed credit for providing treatment for thousands in Botswana, but those figures were later disputed by the Botswanian government.
Certain prerequisites for PEPFAR funding have made its release sometimes difficult. Such prerequisites included drugs that had to be FDA approved, making treatment with unapproved generic brands unavailable; Brazil turned down $40 million because it refused to sign a declaration condemning prostitution; Botswana’s attempts to curb the spread by supplying condoms was stymied by the requirement the condoms go through a lengthy quality-check process even though they had been tested before entering that country. Bush insisted that recipient countries' efforts to curb AIDS must be made through abstinence-only programs instead of safe-sex practices. Many countries with a high HIV/AIDS population also are the poorest countries. Those countries are paying huge interest payments on old and developmentally crippling debts, which further disable them from using their own resources to fight their HIV epidemics.
U.S. involvement in the global problem
In addition to PEPFAR, the U.S. also is the largest donor to the Global Fund to Fight AIDS, tuberculosis, and malaria, at 37.4 percent of the pledges they have received. The Global Fund has dispensed $672 million since its inception in July 2001. USAID, which assists countries recovering from disaster or suffering from poverty, had a budget of $795 million for 2005 and helps 50 countries with HIV/AIDS programs worldwide.
Such private donations as $50 million from the Bill and Melinda Gates Foundation towards the treatment of HIV/AIDS had brought the Global Fund’s total to $150 million by mid-2004. Due to funding shortfalls, however, the Global Fund delayed a fifth round of grants for five months during that year. The Global Fund also receives private donations from such organizations as Bristol-Meyers Squibb Foundations, The Henry J. Kaiser Family Foundation, the Ford and Rockefeller foundations, and other American-based organizations.
With the total number of AIDS deaths between 1981 and the end of 2003 at more than 20 million worldwide, researchers continue to progress along the path to a cure for the aggressively persistent and ever-changing strains of the HIV virus. Many epidemiologists admit a cure for HIV/AIDS is still years away. With worldwide estimates of 39.4 million people living with HIV/AIDS, will the U.S. and other wealthy nations keep pace with funding demands for the prevention and treatment of the disease? Crooked is the road traveled towards a cure, while the spread of HIV/AIDS continues at breakneck speed in some Sub-Saharan African countries and others.